Picture waking up every morning feeling unusually tired, with aching bones and muscles that make simple tasks like climbing stairs feel exhausting. You brush it off as stress or aging, but weeks pass and the fatigue lingers, along with a low mood. This is a common experience for many dealing with low vitamin D levels.
Vitamin D deficiency symptoms often go unnoticed until they affect daily life. This condition happens when your body lacks enough vitamin D, a nutrient vital for strong bones, muscle function, immune health, and mood regulation. Without adequate levels, bones weaken, muscles tire easily, and overall energy drops. It can impact work performance, family activities, and emotional well-being, leading to frustration and reduced quality of life.
Many people worldwide face this issue due to limited sun exposure, diet, or other factors. In this article, you will learn about vitamin D deficiency symptoms, vitamin D deficiency causes, vitamin D deficiency treatment, vitamin D deficiency prevention, and more. These insights come from reliable medical understanding to help you recognize signs early and take responsible steps. Always consult a healthcare professional for personalized advice.
What is Vitamin D Deficiency?
Vitamin D deficiency occurs when blood levels of vitamin D drop too low for the body to function properly. Medically, it is defined as serum 25-hydroxyvitamin D (25(OH)D) below 20 ng/mL (50 nmol/L), with insufficiency often between 20-30 ng/mL.
In simple terms, vitamin D is a nutrient your body needs to absorb calcium and phosphorus for healthy bones and teeth. It also supports muscle strength, immune defense, and brain function. Your skin makes it from sunlight, or you get it from food and supplements.
Low levels weaken bones over time, reduce muscle power, and may affect mood and immunity. For example, someone who stays indoors most days and eats few vitamin D-rich foods might feel constant tiredness and bone aches, showing how deficiency quietly disrupts normal body processes.
Causes and Risk Factors
Vitamin D deficiency causes stem from limited production or intake. Here are the main ones:
- Limited sun exposure: Staying indoors, covering skin, or living in areas with little sunlight reduces skin production of vitamin D.
- Darker skin tones: More melanin blocks UVB rays, so people with darker skin need more sun to make vitamin D.
- Age: Older adults produce less vitamin D from sun and absorb it less efficiently.
- Obesity: Fat cells store vitamin D, making less available in blood.
- Diet low in vitamin D: Few foods naturally contain it; avoiding fatty fish, fortified dairy, or eggs increases risk.
- Medical conditions: Gut issues like celiac or Crohn’s impair absorption; kidney or liver problems hinder activation.
- Medications: Some drugs (like certain anti-seizure meds or steroids) speed up vitamin D breakdown.
- Breastfed infants: Breast milk has little vitamin D without maternal supplementation.
Lifestyle factors like indoor jobs or sunscreen use play a big role. Genetics or environment can add risk, but habits often drive it.
Symptoms and Warning Signs
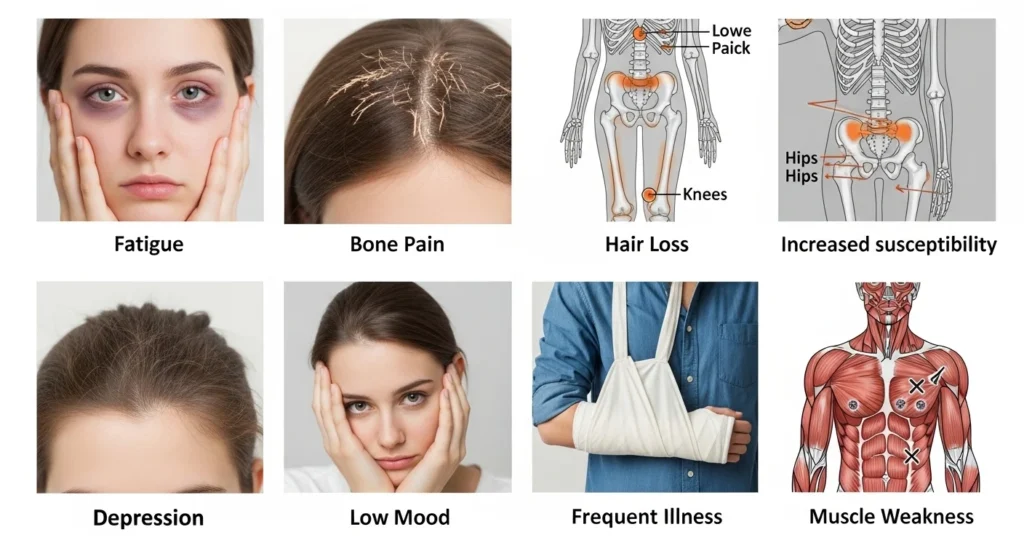
Early vitamin D deficiency symptoms are often subtle:
- Tiredness or fatigue that doesn’t improve with rest
- Muscle weakness or aches
- Bone pain, especially in back, legs, or ribs
- Low mood or feeling down more often
Advanced symptoms include:
- Severe bone or muscle pain
- Frequent falls or fractures from weak bones
- Hair loss or slow wound healing
- Frequent infections due to weakened immunity
In children, it can cause bowed legs or delayed growth. See a doctor if you have persistent fatigue, unexplained bone pain, muscle weakness, frequent illnesses, or mood changes lasting weeks. Blood tests can confirm and guide help.
How It Works in the Body
Vitamin D acts like a key that unlocks calcium use. Here’s the step-by-step process:
- Skin production or intake: Sunlight hits skin to make vitamin D3, or you eat vitamin D2/D3 from food/supplements.
- Liver conversion: The liver turns it into 25-hydroxyvitamin D (25(OH)D), the main measured form stored in blood.
- Kidney activation: Kidneys convert 25(OH)D to active 1,25-dihydroxyvitamin D when needed, like for calcium absorption.
- Action: Active form helps intestines absorb calcium/phosphorus, supports bone building, muscle contraction, and immune cell function.
Think of it as sunlight “charging” your body like a battery for bone and muscle health. Low levels mean poor calcium use, leading to soft bones and weak muscles.
Types / Classification
Vitamin D deficiency is mainly classified by blood levels, not strict types, but effects vary by age and severity.
Nutritional Deficiency
This common form comes from low intake or sun exposure. It leads to rickets in children (soft bones, deformities) or osteomalacia in adults (bone pain, weakness).
Secondary Deficiency
Caused by conditions impairing absorption (e.g., gut diseases) or activation (e.g., kidney issues). It may need specific management beyond sun/diet.
Severe prolonged cases link to osteoporosis (brittle bones) or secondary hyperparathyroidism (overactive parathyroid glands pulling calcium from bones).
Diagnosis and Medical Tests
Doctors diagnose through history, symptoms, and blood tests. The main test measures 25-hydroxyvitamin D (25(OH)D) in blood.
- Blood test results:
- Below 20 ng/mL (50 nmol/L): Deficiency
- 20-30 ng/mL: Insufficiency
- 30+ ng/mL: Generally adequate (some experts aim for 40+)
Other tests may check calcium, phosphorus, parathyroid hormone, or bone markers if needed. Routine screening isn’t for everyone; it’s for those with risk factors or symptoms. Results guide if supplementation or further checks are needed.
Treatment Options
Vitamin D deficiency treatment focuses on raising levels safely.
- Supplements: Vitamin D3 (cholecalciferol) is common; doctors prescribe higher doses for deficiency, then maintenance.
- Lifestyle changes: More safe sun exposure, vitamin D-rich foods.
- Medications: For underlying issues (e.g., treating gut problems).
- Monitoring: Repeat blood tests to track progress.
No surgery is typical. Always get professional guidance to avoid excess, which can cause issues.
Prevention Tips
Vitamin D deficiency prevention involves balanced habits:
- Get 10-30 minutes of midday sun several times a week (arms/legs exposed, depending on skin/location).
- Eat vitamin D sources: Fatty fish (salmon, mackerel), fortified milk/orange juice, egg yolks, mushrooms.
- Consider supplements if at risk (e.g., indoors often); discuss with doctor.
- Maintain healthy weight through activity.
- For infants/children: Follow pediatric guidelines for supplements.
These steps support natural production and intake for long-term bone and overall health.
Advantages and Disadvantages
Advantages of addressing vitamin D deficiency early:
- Stronger bones, fewer fractures
- Better muscle function, less fatigue
- Improved mood and immunity
- Potential lower risk of some chronic issues
Risks of ignoring it:
- Weak bones leading to pain or breaks
- Ongoing tiredness affecting daily life
- Higher infection risk
Pros/cons of treatments: Supplements raise levels effectively with few side effects at proper doses; excess risks high calcium. Natural sources are safe but slower.
Applications / Real-Life Impact
Low vitamin D affects routines: Fatigue reduces work focus or family playtime. Bone/muscle pain limits exercise or chores. Caregivers notice mood dips in loved ones.
Socially, less energy means skipping outings. Emotionally, low mood adds stress. Fixing it restores vitality, confidence, and better daily function.
Common Questions & Practical Solutions (FAQ Style)
Q1: Can vitamin D deficiency be cured?
Yes, most cases improve or resolve with supplements, diet, and sun exposure under medical guidance. Levels rise in weeks to months.
Q2: Is vitamin D deficiency dangerous?
Mild cases aren’t immediately life-threatening but raise risks for bone issues, falls, and weakness. Severe or long-term can lead to serious problems; address early.
Q3: Can it be prevented?
Yes—get regular safe sun, eat vitamin D foods, supplement if needed (especially high-risk groups), and stay active.
Q4: Do I need a blood test?
If you have symptoms or risks, yes. Routine testing isn’t for all; talk to your doctor.
Future Trends and Medical Advances
Research grows on vitamin D’s broader roles. 2025 studies link daily supplements to slower cellular aging (telomere protection) and potential mortality benefits in older adults.
Guidelines (e.g., Endocrine Society) suggest targeted supplementation for children, pregnant people, over-75s, and prediabetes to prevent issues like rickets or infections.
Advances include better understanding of vitamin D in immunity, cancer mortality reduction (12-16% in some meta-analyses for deficient groups), and autoimmune risks. Personalized approaches via testing rise, with focus on daily low-dose over high boluses. Fortification and microbiome links emerge for prevention.
Conclusion
Vitamin D deficiency symptoms like fatigue, bone pain, and weakness signal low levels that affect bones, muscles, and mood. Vitamin D deficiency causes often tie to sun, diet, or health factors, but vitamin D deficiency prevention through sun, food, and habits works well. Vitamin D deficiency treatment with guidance restores balance.
Start by assessing risks and consulting a professional for tests if needed. Small changes bring big benefits for energy and health. Stay aware, act early, and enjoy stronger well-being responsibly.